Translate this page into:
Allergic rhinitis
*Corresponding author: Sowmya A N, Department of Paediatrics, Sanjeevini Clinic and Kangaroo Care Hospitals, Bengaluru, Karnataka, India, 100/2, 11th Cross, Malleshwaram, Bengaluru - 560 003, Karnataka, India. dr.sowmya.nagaraj@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Arudi Nagarajan S, Harsha NS. Allergic rhinitis. Karnataka Paediatr J 2023;38:67-73.
Abstract
Asthma is a chronic airway inflammatory disorder, with variable severity. The mainstay of asthma management is to control symptoms. Sometimes, asthma symptoms will not be controlled in spite of optimal treatment. Many associated conditions such as allergic rhinitis, gastroesophageal reflux disease, obesity, obstructive sleep apnoea, and psychological disturbances are among a few conditions seen concomitantly in patients with asthma, which can directly/indirectly have an impact on the disease process. Influences of comorbid conditions are variable and still uncertain, but many a time alters asthma responses to treatment. Evaluation and appropriate treatment of these comorbidities should be part of asthma management.
Keywords
Asthma comorbidities
Gastroesophageal reflux
Allergic rhinitis
Obesity
Obstructive sleep apnoea
INTRODUCTION
Asthma is an airway inflammatory disorder characterised by airway obstruction. It is of variable severity and is recognised as a spectrum of diseases with varying phenotypes and endotypes, which may impact disease control.[1,2]
The main aim of asthma management is to control symptoms. It is mainly characterised by minimal/no symptoms, no nocturnal symptoms, normal activities, and most appropriate lung function test.[3,4]
Management includes patient education about pharmacotherapy and device use, avoidance measures about environmental triggers with periodic regular follow-ups. Several comorbidities can be associated with asthma as they may be responsible for appropriate disease management.
Asthma in children is unique in that comorbidities were less as compared to adults, but an increasing trend is of concern in recent times. This can impact the quality of life and increase medical expenditure.[5]
These comorbidities are associated with inadequate disease control with impacts the management of the condition.[6] The multipronged approach helps in the identification of these medical conditions, which can ameliorate patient sequelae.[7-9]
Comorbidities are underdiagnosed
Because of increasing awareness of some concomitant conditions such as allergic rhinitis (AR), obstructive sleep apnoea (OSA) is being more frequently diagnosed, than other medical conditions. Hence, we should sensitise peers and patients alike with these conditions.
| Most commonly associated comorbidities with asthma in children |
| Allergic rhinitis Obesity Obstructive sleep apnoea Gastroesophageal reflux Dysfunctional breathing Psychological disturbances (especially depression and anxiety disorders) Food allergy Secondhand smoke exposures |
Possible increased association mainly in adults and adolescents
Chronic rhinosinusitis – mainly in adolescents and adults
Hypertension, diabetes, ischaemic heart disease, and congestive heart disease – mainly in adults
Hormonal disturbances (adult females)
Vasomotor/non-AR
Nasal polyps and aspirin intolerance.
Only Allergic Rhinitis will be covered in detail here.
ALLERGIC RHINITIS (AR)
Rhinitis may be allergic or non-allergic.
Allergies are caused when our body’s immune system reacts to certain substances (allergens) in an exaggerated manner. Allergies can develop at any age. They are more likely to develop if parents and siblings have allergy symptoms. Rarely one may outgrow the allergy over a period of time.
Nearly 20–30% of people in India suffer from allergic conditions including AR and asthma.
Mechanisms
United airway concepts point to the coexistence of upper and lower airway dysfunction.[10] Pathogenesis of AR is described in Figure 1.
![Pathogenesis of allergic rhinitis.[15]](/content/113/2023/38/3/img/KPJ-38-067-g001.png)
- Pathogenesis of allergic rhinitis.[15]
The presence of rhinitis (allergic/non-allergic) increases the risk for asthma.[11] Rhinitis, severity, and sensitisation to allergens are associated with more airway dysfunction and severe asthma.[10,12]
IMPACT OF AR
Impaired quality of life
School absenteeism
Impeded learning
Decreased quality of sleep
Associated asthma, sinusitis, and otitis media.
RISK FACTORS FOR AR
Family history of atopy
Male sex
Early use of antibiotics, in the first 12 months of life
Maternal smoking exposure (passive/active) in the 1st year of life
Presence of allergen-specific immunoglobulin E (IgE).[13]
CLINICAL MANIFESTATIONS
AR can be a combination of sneezing, rhinorrhoea, obstruction of the nose, and or itching. This can present in isolation or a combination of the symptoms mentioned above. In children, postnasal drip can be a presenting feature. Few people also experience itching in the ear or the palate. Many a time, AR can be associated with allergic conjunctivitis, which is overlooked when examining the patient. Always enquire about such symptoms and perform detailed upper and lower respiratory tract examinations.
Acute symptoms may alert the patients of the impairment but chronicity of symptoms may go unnoticed as patients adapt accordingly. Physical findings
Oedema below the eyes and darkening of the skin are referred to as ‘allergic shiners’
Enhanced lines below the lower eyelid margins (Dennie-Morgan lines) can be associated with allergic conjunctivitis simultaneously
A transverse nasal crease on the tip of the nose is caused by repeated rubbing with the hand – ‘Allergic salute’
The nasal mucosa of patients is boggy along with inferior turbinate hypertrophy
Clear rhinorrhoea may be visible anteriorly or postnasal drip.
Immune mechanisms
The World Health Organisation has created a working task force to address the issue of allergic rhinitis and its impact on asthma.[15]
ARIA classification of AR
Allergic Rhinitis and its Impact on Asthma classification is highlighted in Table 1.
 |
Diagnostic tests in AR
In an IgE-mediated reaction; there are the following components to be considered for diagnosis.
Thorough clinical history for possible identification of causative allergens [Table 2]
Tests like allergen skin prick testing (SPT) or in vitro, blood tests (specific IgE immunoassay) will illustrate the presence of allergen-specific IgE.
To determine whether exposure to the causative allergens will result in symptoms, either by history or challenge if needed.
Investigations in AR
Skin prick tests and in vitro-specific IgE tests have many similarities. They demonstrate the presence of allergen-specific IgE, which is the same as saying that he or she is sensitised.
Sensitisation must precede the development of an allergic illness but is not sufficient in itself to justify a diagnosis of an allergy. Relevant history should always corroborate with the results. Skin prick tests are often used as screening tests as the advantages are many. They are cheaper (many allergens can be tested at a single sitting), results are obtained in 20 min and patients can see the results themselves which motivates them to do allergen avoidance measures. Serum IgE testing is the test of choice when:
The patient does not have enough healthy skin for SPT (e.g., severe atopic dermatitis or dermographism)
The patient’s reaction was anaphylactic in the recent past
The patient cannot stop using antihistamines because it causes worsening/recurrence of symptoms.
Skin tests in AR
Skin prick test is usually more sensitive than specific IgE, though there may be a better correlation in the diagnosis of food allergies. Skin prick test may be particularly useful in:
In uncontrolled symptoms in spite of adequate pharmacological treatment
Inconsistent diagnosis based on history and examination
Concurrent lower airway symptoms – Where the patient is willing to do allergen avoidance measures rather than opt for up dosing of pharmacotherapy
SPT should be avoided in symptomatic patients or during peak pollen season (in patients with known pollen allergy), as it can aggravate symptoms. Hence, it is preferred to treat the symptoms and schedule testing once better.
There are certain prerequisites for a skin prick test. The patient must be off antihistamines at least 7–10 days before testing, based on the drug in action, to avoid histamine release necessary for demonstration of Type 1 hypersensitivity reaction to demonstrate degranulation of allergen-specific IgE on cutaneous mast cells
The patient must be well on the day of the test.
Standardised skin prick test allergen reagents are commercially available for many common aeroallergens. The allergen reagent is placed on the skin (usually the volar aspect of the forearm or the back in children) and the skin is pricked through the reagent epicutaneously involving only the dermis. The results are interpreted in 15–20 min. Positive histamine and negative controls are done in the test on each occasion [Figure 2].
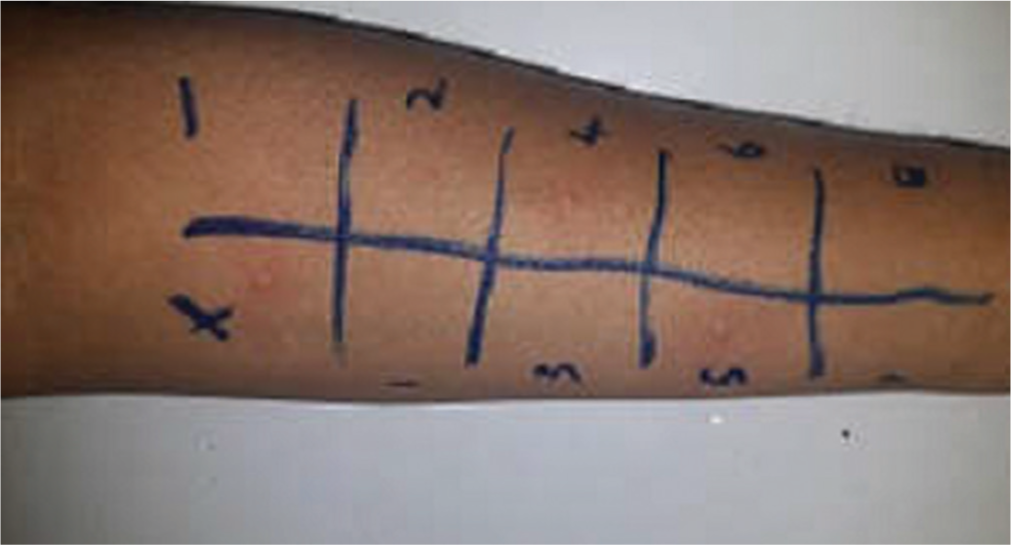
- Allergy skin prick test for aeroallergens with histamine and saline controls.
For interpretation of the test, the wheal (swelling) and flare (redness) responses in 15 or 20 min are recorded. A wheel of >3 mm above the negative control is considered a positive test.
Skin prick tests for aeroallergens generally have better negative predictive value than positive predictive value. The general specificity of these tests is close to 90–95%.
Measurement of allergen-specific IgE
IMMUNOCAP is the standard test done presently to measure serum allergen-specific IgE.[17-20]
Sometimes, we do encounter a patient who has clinical features suggestive of AR, but the allergy test may be negative (both skin testing and in vitro testing). Such patients may be classified as chronic non-AR/or maybe having features of local AR.
Nasal challenges to an allergen or nasal cytology are tests that are limited to research and not routinely used in clinical settings.
In children <2 years of age, other differentials like adenoid hypertrophy, sinusitis, structural abnormalities like choanal atresia, and foreign body have to be considered.
PHARMCOTHERAPY
AR and its impact on Asthma classification will help in the initiation of appropriate pharmacotherapy for patients [Table 3].
| The first line of treatment | Other possible treatments | Short term medications |
|---|---|---|
| Intranasal corticosteroids | Saline treatments | Decongestants (oral or intranasal) |
| Antihistamines (non-sedating-oral or intranasal) | Oral leukotriene antagonists | Systemic oral corticosteroids |
| Combination (Intranasal corticosteroids and antihistamines) |
Intranasal chromones | Combination of intranasal decongestant and antihistamine sprays |
| Intranasal anticholenergics |
The treatment principles include
Treatment can be stepped up or stepped down according to the symptoms. Consistent use of prescribed drugs should be emphasised with proper technique of intranasal steroids [Tables 4 and 5].
Non-sedating antihistamines are preferred as the first line of medication in mild-intermittent AR [Tables 6 and 7].
| Intranasal corticosteroids | First line of therapy recommended for persistent AR |
|---|---|
| Age | Different strengths have different recommendations |
| Frequency | Continuous is recommended, at least for 2–3 weeks. Intermittent-less effective |
| Advantages | 1. Decreases sneezing, itchiness and runny nose 2. Decreases itchy and watery eyes 3. Decreases nasal congestion 4. Cost benefit in long-term |
| Disadvantages | Nasal dryness and occasional nasal bleeding |
AR: Allergic rhinitis
| COMPOSITION OF INS | AGE ALLOWED |
|---|---|
| First-generation | |
| Beclomethasone | 6 years and above |
| Flunisolide | |
| Second-generation | |
| Budesonide | |
| Third-generation | |
| Fluticasone propionate | 4 years and above |
| Fluticasone furoate | 2 years and above |
| Mometasone furoate | 2 years and above |
| Triamcinolone acetonide | 2 years and above |
| Ciclesonide | 6 years and above |
| Budesonide dipropionate | 6 years and above |
| Anti-histamines (second-generation, non-sedating) | |
|---|---|
| Route-oral/intranasal | Rapid onset of action (may be used as a rescue medication |
| Frequency | 1–2 times daily |
| Advantages | 1. Decreases sneezing, itchiness, and runny nose 2. Decreases itchy and watery eyes 3. Limited effect on nasal congestion |
| Disadvantages | Cost |
| Medication | Age range | ||||
|---|---|---|---|---|---|
| 6–11 mo | 12–23 mo | 2–5 year | 6–11 years | ≥12 years | |
| Cetirizine | 2.5 mg OD | 2.5 mg OD/BID Or 5 mg OD | 2.5–5 mg OD | 5–10 mg OD | 5–10 mg OD |
| Levocetirizine | 1.25 mg OD | 1.25 mg OD | 1.25 mg OD | 2.5 mg OD | 5 mg OD |
| Loratadine | - | - | 5 mg OD | 10 mg OD | 10 mg OD |
| Desloratadine | 1 mg OD - | 1.25 mg OD - | 1.25 mg OD | 2.5 mg OD | 5 mg OD |
| Fexofenadine | 15 mg bid (FDA USA) | 15 mg bid (FDA USA) | 30 mg bid | 30 mg bid | 60 mg bid or 180 mg OD |
| Bilastine | - | - | - | - | 20 mg OD |
| Rupatadine | - | - | - | - | 1 tablet (10 mg) once daily |
Correct administration of INS:
Prime the spray device (for the first time or after a period of non-use)
Shake the bottle after each use
Blow nose before spraying if blocked by mucus
Tilt head slightly and gently insert nozzle into the nostril
Aim the nozzle away from the septum (middle) of nose and direct the nozzle into the nasal passage (back or side of the nose)
Avoid sniffing blowing in/out for at least 15–20 min after spraying.
Other treatment options [Table 8]
| Agent | EYE symptom | Itching | Sneezing | Runny nose | Nasal block |
|---|---|---|---|---|---|
| Corticosteroid (Intra nasal) | + | ++ | ++ | ++ | ++ |
| Decongestant (Intranasal) | - | - | - | - | ++ |
| Cromolyn (Mast Cell Stabiliser) | - | + | + | + | + |
| Anti-histamine (Oral) | ++ | ++ | ++ | ++ | +/- |
| Decongestant (Oral) | - | - | - | - | + |
| Anti-histamine (Nasal) | - | + | + | + | +/- |
| Anti-cholinergic (Topical) | - | - | - | ++ | - |
Saline nasal irrigation
Clears the inflammatory mucus and thereby reduces nasal obstruction
Usually well tolerated and acts as an adjunct with pharmacotherapy.
Intranasal chromones (e.g., sodium cromoglycate)
Typically used for mild and intermittent rhinitis
Mainly used for symptomatic treatment. For alleviation of symptoms for a short duration of time
Less effective than intranasal corticosteroids.
Oral leukotriene antagonists
Used in children/adolescents with concomitant asthma and AR
No additional benefit if used in combination with antihistamines for the treatment of AR as it is less effective than intranasal corticosteroids
Recently, FDA has issued a black box labeling of Montelukast as it may cause neuropsychiatric manifestations which are used for a long duration of time. Hence, the cost-effectiveness, duration and probable side effects must be discussed with the family and patient before initiation of the medication.
Decongestants
Oral or nasal decongestants may be used short-term (up to 3–5 days) to reduce nasal congestion if severe
Chronic use of intranasal decongestants may lead to a medical condition called Rhinitis medicamentosa, characterised by rebound nasal obstruction.
Allergen immunotherapy
Allergen-specific immunotherapy – well-defined treatment for IgE-mediated allergic disease
Administered by subcutaneous/sublingual routes
Sublingual immunotherapy, approved in Europe and S America – in process in India; subcutaneous in India,
Allergy immunotherapy-effective treatment for AR
It is the only treatment modality that can change the course of allergic disease and induce allergen-specific immune response
To be considered in patients not controlled by avoidance and medications.
WHEN TO REFER
Patients with persistent or recurrent symptoms, refractory to therapy
Concomitant asthma/sinusitis/polyp
Patients with impaired quality of Life.
Declaration of patient consent
Patient’s consent not required as there are no patients in this study.
Conflicts of interest
There are no conflict of interest.
Financial support and sponsorship
Nil.
References
- Proceedings of the ATS workshop on refractory asthma: Current understanding, recommendations, and unanswered questions. American Thoracic Society. Am J Respir Crit Care Med. 2000;162:2341-51.
- [CrossRef] [PubMed] [Google Scholar]
- Severe asthma in adults: What are the important questions? J Allergy Clin Immunol. 2007;119:1337-48.
- [CrossRef] [PubMed] [Google Scholar]
- Asthma control or severity: That is the question. Allergy. 2007;62:95-101.
- [CrossRef] [PubMed] [Google Scholar]
- Can guideline-defined asthma control be achieved? The Gaining Optimal Asthma ControL study. Am J Respir Crit Care Med. 2004;170:836-44.
- [CrossRef] [PubMed] [Google Scholar]
- Burden of comorbidity in individuals with asthma. Thorax. 2010;65:612-8.
- [CrossRef] [PubMed] [Google Scholar]
- International ERS/ATS guidelines on definition, evaluation and treatment of severe asthma. Eur Respir J. 2014;43:343-73.
- [CrossRef] [PubMed] [Google Scholar]
- Multidimensional Assessment of severe asthma: A systematic review and meta-analysis. Respirology. 2017;22:1262-75.
- [CrossRef] [PubMed] [Google Scholar]
- Profile of difficult to treat asthma patients referred for systematic assessment. Respir Med. 2016;117:166-73.
- [CrossRef] [PubMed] [Google Scholar]
- A structured approach to specialist-referred difficult asthma patients improves control of comorbidities and enhances asthma outcomes. J Allergy Clin Immunol Pract. 2017;5:956-64.e3.
- [CrossRef] [PubMed] [Google Scholar]
- Impact of allergic rhinitis on asthma: Effects on bronchial hyperreactivity. Allergy. 2009;64:439-44.
- [CrossRef] [PubMed] [Google Scholar]
- Perennial rhinitis: An independent risk factor for asthma in nonatopic subjects: Results from the European Community Respiratory Health Survey. J Allergy Clin Immunol. 1999;104:301-4.
- [CrossRef] [PubMed] [Google Scholar]
- The complex link between severity of asthma and rhinitis in mite allergic patients. Respir Med. 2013;107:23-9.
- [CrossRef] [PubMed] [Google Scholar]
- Early-life risk factors and incidence of rhinitis: Results from the European Community Respiratory Health Study--an international population-based cohort study. J Allergy Clin Immunol. 2011;128:816-23.e5.
- [CrossRef] [PubMed] [Google Scholar]
- Allergic and nonallergic rhinitis In: Adkinson NF, Yunginger JW, Busse WW, Bochner BS, Holgate ST, eds. Middleton's Allergy: Principles and Practice (6th ed). St. Louis: Mosby; 2003. p. :1391.
- [Google Scholar]
- Allergic Rhinitis and its Impact on Asthma (ARIA) 2008 update (in collaboration with the World Health Organization, GA(2)LEN and AllerGen) Allergy. 2008;63:8-160.
- [CrossRef] [PubMed] [Google Scholar]
- Skin testing compared with in vitro testing for screening allergic patients. Ann Allergy. 1991;67:133-7.
- [Google Scholar]
- Skin testing versus radioallergosorbent testing for indoor allergens. Clin Mol Allergy. 2005;3:4.
- [CrossRef] [PubMed] [Google Scholar]
- A comparison of different allergometric tests, skin prick test, Pharmacia UniCAP and ADVIA Centaur, for diagnosis of allergic diseases in children. Allergy. 2003;58:38-45.
- [CrossRef] [PubMed] [Google Scholar]
- In vivo methods for the study of allergy In: Adkinson NF Jr, ed. Middleton's Allergy: Principles and Practice (7th ed). Amsterdam: Mosby, Inc.; 2008.
- [CrossRef] [Google Scholar]
- International Consensus Statement on Allergy and Rhinology: Allergic rhinitis. Int Forum Allergy Rhinol. 2018;8:108-352.
- [CrossRef] [PubMed] [Google Scholar]
| ALLERGIC RHINITIS AS A COMORBID FACTOR FOR ASTHMA IN A NUTSHELL • Allergic rhinitis is very common and causes considerable morbidity • Adequate and appropriate treatment leads to significant improvement in quality of life in these patients • Association with asthma is very common, warrants attention in evaluation of patients and appropriate treatment for better control of symptoms. • Intranasal steroids are the first line of recommended treatment in moderate to severe cases • Allergy evaluation and environmental manipulations may also have an important role in the control of disease |







