Translate this page into:
Food allergy: Mechanisms, diagnosis, and management
*Corresponding author: Sowmya Arudi Nagarajan, Department of Paediatrics, Sanjeevini Clinic, Bengaluru, Karnataka, India. dr.sowmya.nagaraj@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Nagarajan SA, Rao HN. Food allergy: Mechanisms, diagnosis, and management. Karnataka Paediatr J 2020;35(2):100-4.
Abstract
Food allergy (FA) is a dynamic field. It is not only evolving but also increasing in the prevalence and incidence all over the world. The term “Food allergy” is often misused, not only by patients, their families but also by health professionals. All adverse food reactions are erroneously labeled as “Food allergy.” This has to be recognized and avoided to make a proper evaluation, diagnosis and management. Surveys have shown that the prevalence of FA based on public perception runs as high as 60%, whereas the true prevalence is around is around 2–8%. FA is more common in early childhood days (6–8%) compared to adults (1–2%). There are several known and unknown reasons for changing picture of FA across the globe. In the developed world, the peanut sensitivity has doubled in prevalence over the past decade. In the developing world (namely, India, and China), the prevalence of Peanut sensitivity/allergy is much less, although the consumption of Peanuts is much higher. Lately, it has also been observed that early introduction of so called “allergenic foods” to infants and children early in life seems to actually reduce the incidence of allergies developing later in childhood.
Keywords
Food allergy
sensitization
Skin prick test
ImmunoCap
Oral food challenge
Definitions
Adverse food reaction: Generic terminology encompassing all untoward reactions to foods
FA: A FA occurs when the body’s immune system sees a certain food as harmful and reacts by causing symptoms. Foods that cause allergic reactions are allergens. It can be immunologic (IgE) (milk, egg, and nuts) or non-immunologic (non-IgE) mediated reactions (celiac disease)
Food intolerance: Metabolic (lactase deficiency)
Food toxicity (food poisoning): Toxins from bacteria, decaying organisms (scombroid fish poisoning).
MECHANISMS OF DEVELOPMENT OF FOOD ALLERGY (FA)
The majority of children do not develop FA. Food allergens are generally weak immunogens. Our gastrointestinal tract by unique mechanisms protects us from developing allergy to multiple food antigens which we ingest daily. Glycocalyx is a sticky lining along the mucosal surface providing the seal between intestinal cells as well as a cementing barrier capable of trapping food particles. This is an efficient barrier system and an essential to maintain the epithelial integrity. In spite of the efficient barrier system, about 2% of ingested food antigens gets absorbed in an immunologically stable form.[1,2]
Oral tolerance
Food antigens are generally weak immunogens. The antigen presenting cells in the GI tract are said to be “non-professional” and are not capable of eliciting a T cell response. The Treg (T regulatory) cells as well as gut flora also play a role in the propagation of oral tolerance. Exclusive breastfeeding also promotes the development of oral tolerance.
Role of gut microbiota
The microbiota inhabiting the normal healthy gut is predominantly Gram negative and shed endotoxin, which through a process activates luminal B cell to preferentially produce IgA and IgG antibodies and thus maintain the integrity of mucosal immunity. On the other hand, disturbance of normal healthy microbiota, that is, dysbiosis, will activate luminal B cells to preferentially produce IgE in place of IgA and IgG and increase susceptibility to allergic diseases.
Early use of broad spectrum antibiotics in 1st year of life and cesarean section will disturb normal healthy microbiota development in gut resulting in dysbiosis and predilection of allergies.
IGE MEDIATED FA
Sensitization to food allergen can occur in two different ways:
The term allergic sensitization describes the first induction of an allergic immune response on allergen encounter. Two routes of allergic sensitization are well established.
Class 1 allergens (e.g., milk, egg, or peanut) are oral allergens that cause sensitization through the gastrointestinal tract.
Class 2 food allergens are mainly allergens in air (e.g., major birch pollen allergen Bet v 1) that causes sensitization through the respiratory tract. These allergens can have cross-reactivity with similar food allergens.
In genetically predisposed individuals, due to the defective epithelial barrier or weak oral tolerance, the food antigens leak through the gut to facilitate sensitization. On re-exposure of the food antigens, specific IgE antibodies residing on mast cells and basophils in the gut bind to the ingested food allergen. This leads to the release of several mediators and cytokines responsible for the clinical cascade of an allergic reaction.
Non IgE mediated FA
A number of non-IgE mediated food hypersensitivity disorders have also been identified. The exact mechanism involved in such disorders is still a matter of debate in certain situations. Non-IgE mediated FA encompasses a wide range of disorders affecting many systems.
Gastrointestinal tract
Food protein induced enterocolitis syndrome (FPIES)
Food protein-induced allergic proctocolitis
Food protein-induced enteropathy
Celiac disease.
Skin
It contacts dermatitis to foods.
COMBINED IGE-MEDIATED AND T CELL-MEDIATED GASTROINTESTINAL DISORDERS
Eosinophilic esophagitis
Diagnostic tests in FA
In an immunoglobulin E (IgE) mediated reaction; there are the following components to be considered for diagnosis.
Thorough clinical history for possible identification of causative allergens
Demonstration of allergen specific IgE by allergen skin prick testing (SPT) or in vitro blood tests (specific IgE immunoassay)
To determine whether exposure to the causative allergens will result in symptoms, either by history or challenge, if needed.
INVESTIGATIONS IN FA
Skin tests and in vitro specific IgE tests share many common properties. They show that the patient harbors IgE antibodies directed against the food allergen, which is the same as saying that he or she is sensitized.
Therefore, specific IgE testing helps to confirm a diagnosis of allergy to a specific food, but is of limited utility if interpreted without or in an inappropriate clinical context.[3]
Skin tests are often preferred to blood testing because skin tests are cheaper (especially when many foods have to be tested), they provide the answer in 20 min and they offer a visual cue to the patient.
Blood specific IgE is indicated only in these instances.
The patient does not have healthy skin for testing (e.g., severe atopic dermatitis or dermographism)
The patient’s reaction was anaphylactic and the doctor is not willing to risk even a skin test; and
The patient cannot stop using antihistamines.
Skin tests in FA
Studies on aeroallergens showed that skin tests are generally more sensitive than in vitro specific IgE test[4,5] though a study on cow’s milk and egg allergy in children showed good correlation between the two.[6]
To reduce the likelihood of a false negative result, patients have to stop using antihistamines before skin testing. The length of time of withdrawal depends on the nature of the antihistamine. For example, long-acting antihistamines such as loratadine and cetirizine should be avoided for 10 days and short-acting ones such as chlorpheniramine and diphenhydramine for 3 days before the test.[7]
Skin test reagents are commercially available for many common food allergens. Another advantage of skin test is its flexibility. The test material is placed on the skin (usually the volar aspect of the forearm or the back in children) and the skin is pricked through the reagent, just penetrating the dermis, and without drawing blood. The reading of the SPT is done in 15–20 min. Positive histamine and negative controls are always included in the test.
In the skin test, the wheal (swelling) and flare (redness) responses in 15 or 20 min are recorded. The positive control must show a strong response and the negative control minimal or no response for proper interpretation. A wheal of >3 mm, equal to or above the positive control is considered as a positive test [Figure 1].[8,9,10]
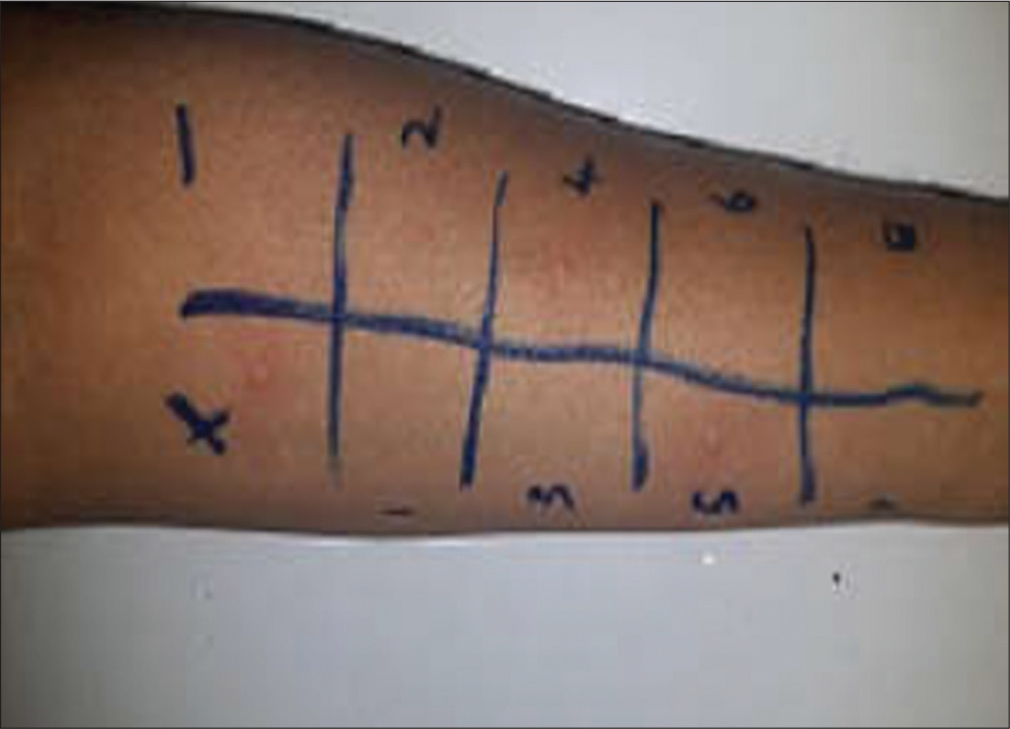
- Allergy skin prick test for foods with histamine and saline controls.
Measurement of allergen-specific IgE
Radioallergosorbent test was the usual way of performing this test, but enzyme methods (e.g., fluorescent enzyme immunoassay, and FEIA) are more commonly used now.[8]
It is better to wait for 4–6 weeks to elapse after an IgE-mediated hypersensitivity reaction before assaying the specific IgE concentration because the IgE is consumed during the reaction, and therefore, may be falsely negative. The concentration of specific IgE is reported in terms of classes, even though modern equipment is capable of providing a precise quantitative result.
ORAL FOOD CHALLENGES (OFC)
OFC are performed by feeding the patient the suspected food under physician observation.
There are several situations in which physician –supervised OFC are required for diagnosis of food allergic disease.
In general when several foods are under consideration as a cause of symptoms, tests for specific IgE are positive, the positive predictive value of a positive ST for food is only 50%. Hence, it might be necessary to conduct an oral challenge to decide regarding reintroduction of food item
If tests for specific IgE false positive, challenges may be only way of diagnosis
Oral challenges are also an integral part of following patients likely to lose their clinical reactivity to the food in question. Since skin test may remain positive for years following the achievement of clinical tolerance to a particular food, OFC are often the only means to determine whether the allergy has been “outgrown”
OFC are strictly to be done in a setting equipped to deal with severe allergic reactions as these reactions can be expected and should be appropriately dealt with.
Diagnosis of Non-IgE mediated food allergies
Diagnosis made by allergist or gastroenterologist
It is easily misdiagnosed: Because it is not your typical FA as symptoms are not immediate and do not show up on standard allergy tests as described above or in biopsies, unless IgE also present as in atypical FPIES.
Blood tests during acute reaction mimic the body’s response to infection.
Atopy patch testing is not validated but may be helpful in delayed reactions.
It may present acutely or chronic and mimic other disorders of infancy, additional symptoms secondary to reactions may be present (making it more difficult to pinpoint diagnosis).
OFC is the most definitive test, however, not often needed initially if the doctor has excluded other diagnosis and the medical history is consistent with the diagnosis.
Present research in FA
As the focus has been shifted to the prevention of infections in keeping the environment more sterile and minimalist interaction between human, animals, and microbiota, it has seen the surge of allergic diseases since late 1990s. There has been an increased emergence of food allergies in the past two decades with awareness of common foods causing FA. At present, the research focus is on treatment and any measures which can help in prevention of food allergies.
Even though few studies, initially have shown some promising results of bacterial products in preventing atopic dermatitis and augmentation of sustained oral tolerance in food oral immunotherapy (OIT),[11] not all studies have been promising. At present, there are no recommendations for use of microbial products in the treatment or prevention of FA by the world allergy organizations.
The earlier recommendations of highly allergenic food avoidance in the west were withdrawn as studies failed to show beneficial effects of the same.
The learning early about peanut allergy (LEAP) study[12] from United Kingdom was a very interesting study, which involved high risk babies (with egg allergy, eczema, or both) who were randomized to two groups of peanut consumption and peanut avoidance. They reported that in the peanut consumption group, at risk of developing peanut allergy, showed a marked reduction of odds of 70–80% of peanut allergy. This has led to re-work on guidelines endorsing age appropriate weaning foods and no role of avoidance of highly “allergenic” foods, which are essential for nutrition of a growing child.
A lot of research has been ongoing with promising results, to impart of sustained immune tolerance to allergenic foods by consumption of these foods in desensitization to foods by OIT or sublingual immunotherapy. Tolerance implies that the food can be ingested without the appearance of allergic symptoms despite periods of withdrawal.
There has been promising evidence on adjuvant of omalizumab with multiple food allergen OIT and has been shown to reduced time (about 67 weeks) taken for developing tolerance to these foods in Phase 1 of these trials, saving them about 67 weeks’ worth of time if they had undergone desensitization to individual foods.[13] There are some outstanding issues with OIT. Uncontrolled nature of most of the trials, different parameters included in the methods and heterogeneity in protocols is to name a few. However, the time may be ripe for the practice of OIT in clinical practice in the coming years.
In conclusion, as we are encountering increased prevalence of FA as a part of Allergic March, time has come to build on available knowledge and to set up new studies which can provide us more armor in the near future.
Quick pointers
In the clinical scenario, the emphasis is still on a good clinical history and examination, demonstration of IgE-mediated reaction with correlated ingested foods either with SPT or in vitro testing, patient education about avoidance of causative foods and treatment of allergic reactions
The attending medical practitioner must take into account the context in which he or she practices and the patient’s condition when choosing between skin testing and in vitro specific IgE testing
SPT are safe, fast, inexpensive (as compared to serum specific IgE) and easy to perform. It can be safely performed even in the infancy with minimal risk. It is better performed by personnel trained with the technique. It has moderate to good correlation (with sensitivity of 50–60% and specificity of 80–90%) with the serum specific IgE in food allergies. This is reassuring for patients with contraindications/access to either test as the results will likely match[14]
The practitioner should not order a large number of specific IgE tests to screen for allergy when the diagnosis of IgE-mediated FA has not been established
The common foods causing food allergies include milk, egg, wheat, fish, and peanut among others. Therefore, usually SPT to about 8–10 foods will be able to diagnose majority of food allergies
All the tests will have to be interpreted in the context of clinical history, which should drive the advice on avoidance of particular foods, rather than blanket avoidance of foods. Misconceptions about FA exists because of correlation of a positive test result to a particular food (either by SPT or serum specific IgE) to having a FA[15]
OFC are the gold standard for the confirmation of a FA. In a majority of cases, combination of accurate history and allergy testing (either by SPT or serum specific IgE) can accurately diagnose or exclude FA. OFC may be needed only when the history or test results or both are inconclusive[15]
Food allergies can cause anaphylaxis, if not recognized and treated, can be life-threatening. Use of intramuscular epinephrine (0.3 mg for adults and children above 30 kg, 0.15 mg for children <30 kg, and with repeat dose if needed) should not be delayed in such instances, along with supportive management. Subsequent testing for food allergens must be deferred until 4–6 weeks
Even though there are promising results in the role of probiotics in prevention or augmenting the desensitization or OIT process from few clinical trials, there are yet currently no recommendations for its use in clinical practice by World Allergy Associations
In view of results of LEAP study and similar ones, there is more emphasis on introduction of age appropriate weaning foods in the west. It can be attributed to the same fact that FA is less prevalent in the Indian scenario as age appropriate weaning foods are traditionally followed in Indian households
There is no role for testing serum total IgE/absolute eosinophil count/total IgG4 levels in the diagnosis of food allergies as it does not give any useful information regarding the diagnosis, prognosis, or management
Children with moderate to severe atopic dermatitis may benefit from investigations to assess for FA. The investigations must be interpreted in context and confirmed with food challenges and, if necessary, food avoidance. In most situations, these tests should be carried out by specialists experienced in treating food allergies
Specific foods such as banana, citrus foods are incriminated in aggravation of concomitant respiratory conditions such as asthma or allergic rhinitis. It may be because of increase in naturally occurring histamine in these foods, which may act as triggering of an acute exacerbation.
It may also be related to oral allergy syndrome, which occurs in patients with allergic rhinitis with pollen sensitization. In these patients, eating of foods which are cross reactive to certain pollens, they cause tingling sensation or itching in the oral cavity but do not cause any systemic symptoms.
Hence, advice for unnecessary avoidance of foods must be given with discretion to parents, bearing in mind, that this can cause micronutrient deficiency in children, if done without proper scientific reason.
Declaration of patient consent
Patient’s consent not required as patients identity is not disclosed or compromised.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Available from: https://www.foodallergy.org/facts-and-stats [Last accessed on 2020 May]
- Randomized trial of introduction of allergenic foods in breast-fed infants. N Engl J Med. 2016;374:1733-43.
- [CrossRef] [PubMed] [Google Scholar]
- Interpretation of tests for nut allergy in one thousand patients, in relation to allergy or tolerance. Clin Exp Allergy. 2003;33:1041-5.
- [CrossRef] [PubMed] [Google Scholar]
- Skin testing compared with in vitro testing for screening allergic patients. Ann Allergy. 1991;67:133-7.
- [Google Scholar]
- Skin testing versus radioallergosorbent testing for indoor allergens. Clin Mol Allergy. 2005;3:4.
- [CrossRef] [PubMed] [Google Scholar]
- A comparison of different allergometric tests, skin prick test, pharmacia UniCAP and ADVIA centaur, for diagnosis of allergic diseases in children. Allergy. 2003;58:38-45.
- [CrossRef] [PubMed] [Google Scholar]
- In vivo methods for the study of allergy In: Adkinson NF Jr, ed. Middleton's Allergy: Principles and Practice (7th ed). Amsterdam: Mosby, Inc; 2008.
- [CrossRef] [Google Scholar]
- Practice parameters for allergy diagnostic testing, Joint Task force on practice parameters for the diagnosis and treatment of asthma, The American academy of allergy, asthma and immunology and the American college of allergy, asthma and immunology. Ann Allergy Asthma Immunol. 1995;75:543-625.
- [Google Scholar]
- In vitro assays for the diagnosis of IgE-mediated disorders. J Allergy Clin Immunol. 2004;114:213-25.
- [CrossRef] [PubMed] [Google Scholar]
- Skin prick test sensitisation patterns in children and adults presenting with allergy symptoms in bangalore-A retrospective analysis. Int. J. Curr. Adv. Res. 2017;6:2399-404.
- [CrossRef] [Google Scholar]
- Administration of a probiotic with peanut oral immunotherapy: A randomized trial. J Allergy Clin Immunol. 2015;135:737-44.
- [CrossRef] [PubMed] [Google Scholar]
- Randomized trial of peanut consumption in infants at risk for peanut allergy. N Engl J Med. 2015;372:803-13.
- [CrossRef] [PubMed] [Google Scholar]
- Phase 1 results of safety and tolerability in a rush oral immunotherapy protocol to multiple foods using omalizumab. Allergy Asthma Clin Immunol. 2014;10:7.
- [CrossRef] [PubMed] [Google Scholar]
- Retrospective analysis on the agreement between skin prick test and serum food specific IgE antibody results in adults with suspected food allergy. Allergy Asthma Clin Immunol. 2016;12:30.
- [CrossRef] [PubMed] [Google Scholar]






